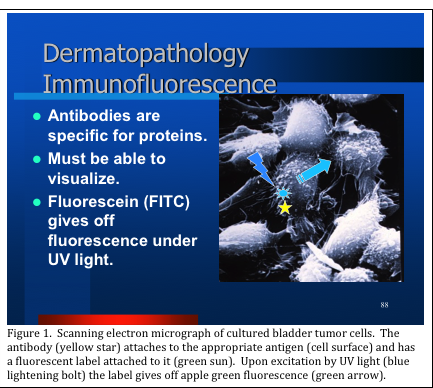
There are some pathological conditions that exist that cannot be accurately diagnosed by examining hematoxylin and eosin (H&E) stained slides alone. In such cases, the pathologist may order immunohistochemical (IHC) stains to help render a diagnosis. Immunohistochemical stains are classified as either immunofluorescence (IF) or immunoperoxidase; however both make use of highly specific antibody preparations to detect their specific antigens in tissue sections. Direct immunofluorescence (DIF) utilizes a fluorescent label attached directly to the antibody. Upon viewing under ultraviolet (UV) light in a dark field microscope, the label fluoresces an apple green color (Figure 1).
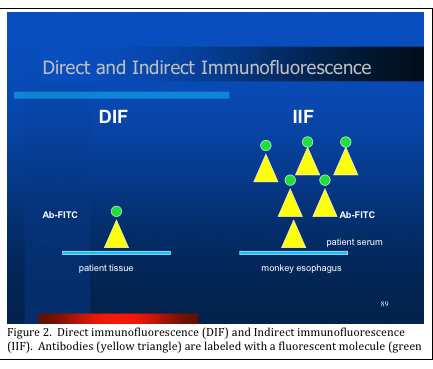
Immunofluorescence is further classified into direct immunofluorescence (DIF) or indirect immunofluorescence (IIF). This procedure is done for patients who present with bullous (i.e. blistering) disease, which may have an autoimmune cause. DIF is done by cutting frozen sections of the patient’s skin specimen, and then incubating these slides with specific fluorescein labeled antibodies. IIF makes use of the patient’s serum, serially diluted and incubated on substrate slides (i.e. frozen sections of monkey esophagus). A second fluorescein labeled antibody is then applied. The resulting slides of both DIF and IIF procedures are then viewed in a dark field fluorescence microscope and the pathologist records the resulting staining patterns to make an accurate diagnosis Figure 2).
Immunoperoxidase stains are performed on sections of formalin fixed paraffin embedded tissue (i.e. the identical material from which the H&E slide is made from). Sections are cut, baked and then hydrated to stain either manually or with automated technology. The resulting specific chromogen stain can be viewed under regular light microscopy. Whether or not a particular antigen is present helps the pathologist to make an accurate diagnosis.
Immunoperoxidase (IP) methods are based on the same mechanism as IF methods. Specific antibodies are used to detect and bind to specific antigens located within the tissue section. These antigens may be proteins located on the exterior of the cell, within the interior of the cell, on the cell membrane, on the nuclear membrane, or within the nucleus. [There are even other, in situ methods, that can detect gene aberrations within the nucleus. We will explore these methods in a future blog.]
Antibodies themselves are too small to be seen under a microscope. So, like the IF procedures, the IP procedures employ methods to “label” the site of antibody: antigen binding. Figure 3 is a schematic representation of the IP method. The primary antibody binds to the antigen present in the tissue section. A secondary antibody, labeled with a link (either a biotin or polymer link) is applied, and binds to the primary antibody. The final detection molecules are added, and bind to the link reagents. These detection molecules form colored precipitates at the site of antibody binding when they are developed. Final reaction products can be brown, red or blue, depending upon the chromogen used (Figure 4).
An important detail is that specimens for DIF must be collected into a specific immunofluorescence transport medium, such as Michel’s medium, in the clinicians’ office. The specimens must then be recognized when they arrive in the histology laboratory and routed to the immunohistochemistry laboratory. At no time can these specimens be exposed to formaldehyde. Formaldehyde exposure renders these specimens unsuitable for immunofluorescence.
Detection of protein antigens within tissues and cells assists the pathologist in making accurate diagnoses. This is especially important when the diagnosis cannot be made entirely with the H&E slide. The results may also be used in determining how to treat the patient.

REFERENCES:
Theory and Practice of Histological Techniques. JD Bancroft, A Stevens ed. Churchill Livingstone, NY. Fourth edition. 1996
Theory and Practice of Histotechnology. DC Sheehan, BB Hrapchak. CV Mosby Company, St. Louis. First edition. 1980.